Home » Cholangiocarcinoma
Cholangiocarcinoma
About Cholangiocarcinoma
Cholangiocarcinoma is a gallbladder and biliary tract cancer and is the second most common liver tumor. The disease is created when cancer cells develop in the tissues that build the gallbladder and the biliary tract.
The cancer develops in a small liver tube that carries the bile and reaches the gallbladder. Bile duct cancer accounts for 10-20 percent of all liver cancers.
This is an aggressive cancer, as most patients are diagnosed with advanced disease, where the disease is usually incurable.
The life expectancy of the patient is bleak and lasts for about 3 years, with the support of the standard treatments.
To improve patients’ chances, the American Society for Clinical Oncology, ASCO, that includes various specialists in its panel, such as oncologists, radiologists, gastrologists among others, guides oncologists to inform Cholangiocarcinoma patients in all topics related to clinical trials in every stage of their disease.
The National Cancer Institute, NCI, of the United States, stresses that for part of Cholangiocarcinoma patients, the preferred treatment option is to join one of the many clinical trials around the world and thus increase the chances of success over the standard protocols.
Types of Cholangiocarcinoma
This cancer is divided into three subgroups:
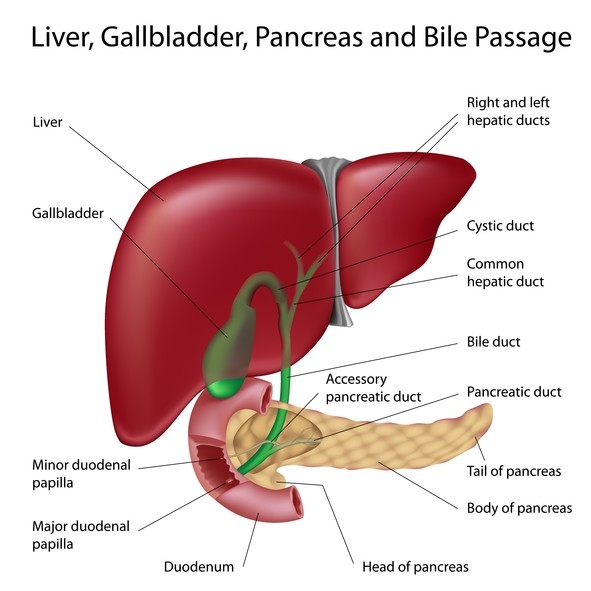
- Intrahepatic cholangiocarcinoma – Tumors that occur in the bile ducts inside the liver
- Extrahepatic cholangiocarcinoma – Tumors that occur in the bile duct outside the liver
- Tumors that occur in the site where the biliary tract come out of the liver. Tumors that occur at the site of the junction between the left and right hepatic tracts and form the hepatic duct are called “Klatskin tumor”.
Risk Factors
- Hepatitis B or C
- Alcoholism
- The history of biliary tract infections
- Congenital cyst in the biliary tract
- Caroli disease – An innate rare disease of small bile duct size. This syndrome raises the style of infection and stones, such as gallstones, form in the liver.
- Cirrhosis of the liver – Cirrhosis is a liver disease to say to cause scars or irritation over time. Cirrhosis can have many causes and most often comes from excess alcohol and viral hepatitis, hepatitis C, style C
Cholangiocarcinoma Symptoms
- Jaundice – yellowing of the skin and white of the eyes
- Itchy skin
- Losing weight without trying to lose weight
- Loss of appetite
- Fever
- Upper abdominal pain
- Nausea and vomiting
- Weakness and fatigue
- Dark urine
Treatment Goals
The goal of treating local cancer, not metastatic, is to remove and eradicate the tumor completely.
In metastatic stage 4 disease, the primary objective of the treatment is to slow down and control disease progression and help reduce symptoms as well prolong life and improve patient’s quality of life.
Standard Treatments
A number of therapies are possible, and many patients shall receive more than one type of therapy. Treatment options for liver cancer depend on several factors, like a patient’s overall health, how much liver damage has been caused by cancer, hepatitis or cirrhosis and whether the cancer has spread.
Surgery
The purpose is to remove the tumor and the area adjacent to it. The tumor will be studied under the microscope to identify and diagnose the type of cancer.
Two main types of treatment may be offered to patients before and after surgery
-
Treatment prior to surgery is known as ‘Neoadjuvant’
Usually this stage of treatment will involve chemotherapy and/or radiotherapy intended to reduce the tumor’s size and improve the success of surgery.
-
Post-surgery treatment, also known as ‘Adjuvant’
This treatment seeks to cure and prevent the appearance of metastases or recurrence of the tumor.
Ablation
Ablation is treatment that aims to destroy tumors in the liver without taking them out. These techniques can be used in patients with a few small tumors and when surgery is not a good option. They are less likely to cure the cancer than surgery, but they can still be very helpful.
Ablation is best used for tumors no larger than 3 cm across. Because ablation often destroys some of the normal tissue around the tumor, it warrants special consideration in certain cases depending on the location of the tumor.
Often, ablation can be done by inserting a needle or probe into the tumor through the skin. The needle is guided into place with ultrasound or CT scan.
Whipple Procedure, Pancreaticoduodenectomy
Surgery to remove the infected part, along with part of the pancreas, small intestine (duodenum), gallbladder and biliary ducts and lymph. The surgery is possible when the tumor is relatively small and not spread.
This is a surgery to remove the cancerous part with the aim of not injuring all the liver and preserving its normal function as much as possible.
Complete removal of the tumor can ensure rapid recovery.
Unfortunately, Cholangiocarcinoma is most commonly found when the cancer cells have already spread to other organs and have metastasized. In this condition, the patient is defined as “not-resectable” and stage of disease is stage 4, metastatic.
Radiation
Radiation therapy for cancer in the liver uses targeted energy, similar to an X-ray, to destroy cancer cells, shrink tumors and/or relieve symptoms while reducing exposure and damage to normal, healthy tissue.
Clinical Trials
For patients looking to continue to treat cancer, participating in clinical trials with newer treatments and advanced medications may be a very good treatment option. In this way, patients can receive the best treatment currently available and may also receive the treatments that are considered even better.
Patients can enter clinical trials before, during, or after starting cancer treatment. There are several clinical trials that include only patients who have not yet been treated. Other trials are investigating treatments for patients whose cancer has not improved. There are also clinical trials investigating new ways to stop the recurrence or reduce the side effects of cancer treatment.
Clinical trials are taking place all over the world and must be screened to the patient’s clinical data and medical background.
Cancer is called “recurrent” when it recurs after treatment, or in other words, the treatment had failed. The recurrence of the cancer can be local – in the same place where it started or near it, or distant – when the cancer appears in other organs of the body, such as the lungs. This is stage 4, metastatic.
If the cancer recurs, further treatment depends on where it returned, the type of treatment the patient has received in the past and the general health of the patient.
In most cases, if the cancer returns after the initial treatment, it will not be possible to go back and the treatment will be aimed at controlling the growth of the cancer and alleviating the symptoms. In rare cases, if the cancer recurs where it started, surgery to remove the cancer (and perhaps subsequent treatment) may be a possibility.
But because most recurrent cancers are incurable, patients want to consider taking part in clinical trials with newer treatments and advanced drugs.
Liver Transplant
In a liver transplant, the entire liver is removed and replaced with donated healthy liver. Liver transplantation may be performed in Perihilar Cholangiocarcinoma patients. If the patient has to wait for a liver donation, another treatment is considered.
Chemotherapy
Before surgery to destroy cancer cells and shrink tumors
After surgery to target cancer cells that may have been left behind
As a systemic treatment to treat locally advanced or metastatic liver cancer
The most common chemotherapy drugs for treating liver cancer include:
- Gemcitabine (Gemzar)
- Eloxatin®, (Oxaliplatin)
- Cisplatin
- Doxorubicin (pegylated liposomal doxorubicin, Doxil®)
- Adrucil®, (Fluorouracil, 5-FU)
- Xeloda®, (Capecitabine)
Sometimes, combinations of 2 or 3 of these drugs are used.
Biological Drugs
Those drugs specifically bind to unique biomarkers like receptors and proteins that feature the individual cancer cells. Once attached to targeted cancer cells, the drugs work by either killing the cells or helping other therapies, such as chemotherapy, identify and target cancer cells.
Under this category, you may find:
- Sorafenib (Nexavar®)
- Lenvatinib (Lenvima®)
- Regorafenib (Stivarga®)
- Cabozantinib (Cabometyx®)
- Ramucirumab (Cyramza®)
Targeted Drugs
The more researchers study and learn about genetic changes and proteins in cancer-causing cells, the more they develop newer drugs that specifically target these changes and proteins. A targeted drug is used to treat many cancers. Many of these drugs are being tested to see if they can help in the treatment of Cholangiocarcinoma. Currently, the only way to get these drugs is through clinical trials or compassionate request.
Targeted drugs work differently from standard chemotherapy drugs, chemo’. They often work when regular chemical drugs are not, and often have different side effects than chemo and less severe.
They can be used with or without chemotherapy.
Immunotherapy
Immunotherapy drugs assist the immune system in attacking the tumor. This type of treatment is very different from chemotherapy, for example, which directly attacks the cancerous cells but unfortunately also damages healthy tissues.
The immune system has “immune barriers” which serve to regulate the immune system and prevent it from attacking the body. In cancer these functions are readily activated and as a result, the immune system ceases to attack cancerous cells, enabling the tumor to grow and proliferate in the body.
Barriers known as PD-L1, PD-1 and CTLA-4 are found on T-cells and cancer cells.
Immunotherapy is a revolutionary strategy, and one of the most widely studied worldwide for its application to numerous types of cancer and various stages of the disease’s development. Treatment is generally provided in the form of an intravenous infusion.
Many of these drugs are being tested in clinical trials to see if they may help in the treatment of Cholangiocarcinoma.
 Advanced Cancer Drugs and Breakthrough Treatments in Clinical Trials Around the World for Cholangiocarcinoma
Advanced Cancer Drugs and Breakthrough Treatments in Clinical Trials Around the World for Cholangiocarcinoma
Facts
- The existing therapies used on stage 4 metastatic liver cancer are not curative, and this is a source to the need for innovative and effective treatment strategies in order to fight the disease.
- The National Cancer Institute, NCI, highlights the fact that for a certain group of liver cancer patients, the best treatment option is to join one of the many clinical trials existing worldwide aiming to increase their chances of therapeutic success.
- Currently, every patient will be offered the standard protocols described above. Sometimes the oncologist may suggest integrating these therapies with trials carried out in the institute.
The Opportunity
- Advances in cancer therapies may be found in clinical trials prescribing cutting edge, innovative drugs, some of which have already been recognized by the US Food & Drug Administration, the FDA, as “breakthrough drugs” and require further information to be approved.
- An entire world of clinical trials, Compassionate drugs and advanced new cancer treatments are available worldwide.
- It is important to know and have access to cutting edge cancer treatments that best match the unique medical condition of the patient and increase chances in winning the fight against compared to the standard care offered.
Note to remember!
Not every patient is eligible to enter a specific clinical trial. The eligibility conditions must be fully met and each case is reviewed separately to ensure that the clinical trial matches to the specific cancer patient and vice versa.
References
ttps://www.fda.gov
https://www.ema.europa.eu
https://www.health.gov.il
https://www.cancer.org
https://www.cancerresearchuk.org
https://www.cancerresearchuk.org
Dear Reader,
This information is provided as a source of knowledge and does not constitute a medical consultation. For professional medical advice, see your attending physician. Information regarding drugs and commercial names belongs to the pharmaceutical companies.
To check if our service suits your case
We need to talk

Improve therapeutic outcomes, prolong life and quality of life, are our main business.
We support access to and expand cancer treatments beyond the standard of care, with the most advanced and innovative treatment options in the world, personally matching the individual cancer patient’s medical condition and with the support of top tier oncologists.
Article categories
קטגוריות המאמרים
Popular topics






